Hilo Medical Center full amid latest COVID-19 surge
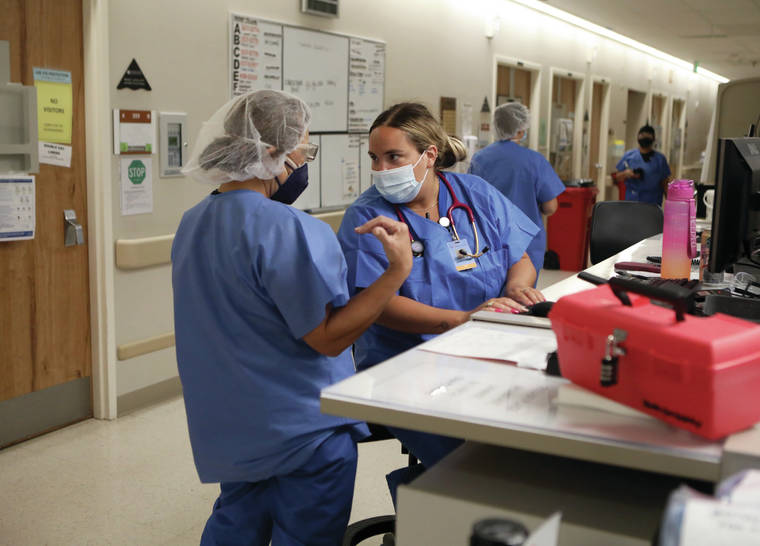
Kelsey Walling/Tribune-Herald Christina Perez, right, speaks with another COVID-19 nurse while working Tuesday on patient paperwork in the COVID-19 unit at Hilo Medical Center.
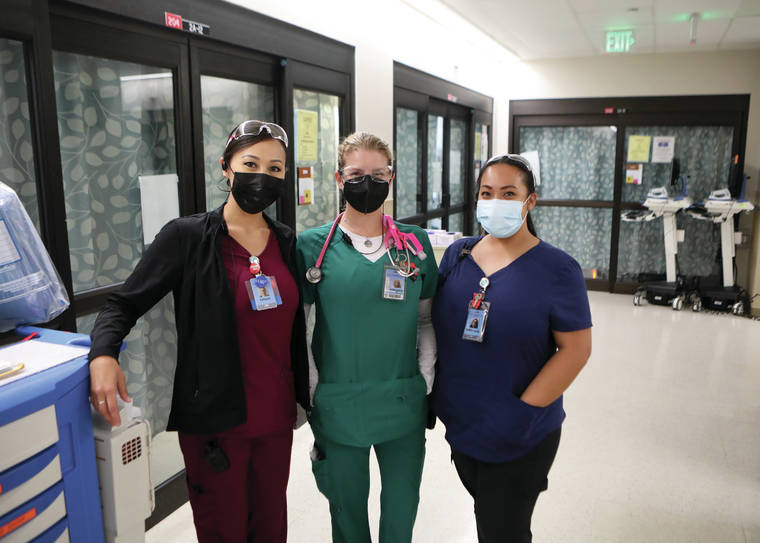
Kelsey Walling/Tribune-Herald From left, Tiffany Martinez, Amanda Wagenblast and Mary-Ann Calamayan stand together Tuesday in the ICU at Hilo Medical Center.

Kelsey Walling/Tribune-Herald Christina Perez removes a face shield after helping a patient in the COVID-19 unit at Hilo Medical Center on Tuesday, Aug. 10, 2021.

Kelsey Walling/Tribune-Herald Sarah Tai gets her eye protection Tuesday before entering a COVID-19 patient's room in the ICU at Hilo Medical Center.
Tiffany Martinez, an intensive care unit nurse at Hilo Medical Center, has been working with COVID-19 patients since the onset of the pandemic 17 months ago.
Tiffany Martinez, an intensive care unit nurse at Hilo Medical Center, has been working with COVID-19 patients since the onset of the pandemic 17 months ago.
“I think it can be disheartening to be here,” she said Tuesday. “We’re not only taking care of active COVID cases up here, but people who remain sick after COVID leaves their system. They are still here because they are so sick.”
ADVERTISING
The recent surge of COVID-19 is straining the capacity of hospitals across the state — including those on the Big Island.
“We’ve had to send ICU nurses to the ER because there isn’t always enough room to bring people up here,” Martinez said. “We only have an 11-bed ICU, so there is a worry that we could be overrun.”
Indeed, all 128 acute and intensive care beds at Hilo Medical Center were full Tuesday.
HMC spokeswoman Elena Cabatu said hospital beds remain full in part because the hospital cannot transfer patients out to long-term care facilities, many of which are not currently accepting new patients amid the virus surge.
There will be an occasional “moment of breathing room,” she said, “but it’s a moment, because we will fill (the beds) up.”
According to Cabatu, 10 COVID-19 patients were hospitalized as of Tuesday afternoon.
“We are still seeing them between the ages of 20 and 50,” she said. “That reflects the low vaccination rates among that age group.”
While HMC has treated “breakthrough” cases — or COVID-19 in people who have been fully vaccinated — Cabatu said only two fully vaccinated individuals have been hospitalized, “and they only stayed for a few days.”
Two active and three long-term patients occupied five of the hospital’s 11 ICU beds Tuesday.
“What we’re seeing on average is COVID patients are staying with us for four weeks, and non-COVID patients stay with us four days,” Cabatu said.
One coronavirus patient has been there more than 90 days.
If there was any doubt about the presence of long-term COVID, Cabatu said, “it is here, and it is real.”
As health care facilities reach capacity, Cabatu said all hospitals are considering expanding their “surge capacity.”
“(We) looked at that at the beginning of the pandemic, seeing where we can open more beds.”
The hospital can find the capacity, Cabatu said, but the bigger problem is an already “stretched and strained” staff.
“Over the last year, as the pandemic has gone on, a lot of nurses migrated out of the clinical nursing roles,” Cabatu said.
Front-line workers are tired, she said.
But when it comes to finding respite, Cabatu said contrary to last year, hospitals across the country now are seeking the same help at the same time.
“Deploying help was a lot easier last year because (you) could deploy nurses and providers to hotspots, where now you look at the map (and) almost everywhere is a hot spot.”
Gov. David Ige shared similar sentiments during a news conference Tuesday, and said the state is working to bring in additional health care staff to assist.
“We are fully aware of the staffing shortage and are working with the Healthcare Association of Hawaii and all of the facilities to make arrangements to bring in additional nurses and other medical technicians and staff,” he said. “We are projecting to contract with up to 500 health care professionals to help through this surge.”
The state also has applied to the Federal Emergency Management Agency for additional health care support.
“So, we have plans. We’ve anticipated the situation that we see coming, and all of the hospitals are implementing (surge plans) to ensure that we have space for those who need care,” Ige said.
Christina Perez, a travel nurse working in HMC’s COVID-19 unit, is nearing the end of a three-month stint in Hilo.
“As a travel nurse, I’ve been working in COVID-19 units across the country,” she said. “This definitely iasn’t the worst experience I’ve had, but this month has been really hard. The numbers were really good here, and now it’s declining, which is hard to see.”
Photojournalist Kelsey Walling contributed to this story.
Email Stephanie Salmons at ssalmons@hawaiitribune- herald.com.